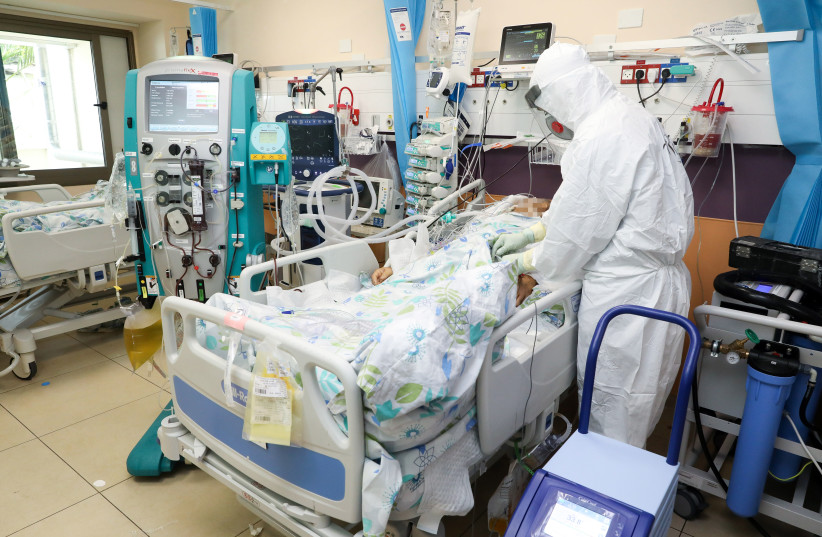
Medical and nursing school students are regularly instructed that communicating with patients’ families is important if they want to understand the person’s background and medical history, as well as their loved ones’ involvement and feelings toward prognosis.
But an internal medicine team at Sheba Medical Center at Tel Hashomer and Tel Aviv University’s Sackler Faculty of Medicine has cast doubt on the practice of allowing family members to accompany medical staffers on their rounds when visiting the patient. Writing in the latest issue of the Israel Medical Association Journal (IMAJ), Drs. Maya Yakir, Adi Brom, Amitai Segev, and Gad Segal say that this can lead to worse clinical outcomes.
“One approach that facilitates the improvement of this communication is the assimilation of family-centered rounds into the daily routine of the internal medicine department,” they wrote. But data on any benefits from this are very rare. Previous studies have shown that 85% to 100% of families actually preferred that when given the opportunity, they would like to be with the medical staff during rounds at their loved one’s bedside.
Emergency staffers did not support family involvement in all cases
Studies have shown that most emergency department staffers opposed family presence during resuscitation, mostly due to worries about being criticized by the family, being exposed to lawsuits and fear of hurting their feelings.
The Sheba team looked at all patients admitted for three to seven days – the average stay in the internal medicine departments during one year. One group had no family members present at rounds; another had them present at up to three-quarters of doctors’ visits and the third who were there during more than 75% of rounds. They looked at mortality rates, re-hospitalization, personal status of family members and more.
The team found that increased family member attendance was associated with negative clinical outcomes and higher long-term death rates, as well as the likelihood that the patients had to return to the hospital ward later. It was even linked to an increased incidence of delirium events in the hospital.
“The present findings do not demonstrate a definitive causal relationship between family member attendance and prognosis,” they concluded, “but at the present time, our results do not give reasons to encourage such attendance.”