Many people suffering from hearing loss refuse to get hearing aids because of embarrassment or their refusal to accept the fact that have a disability. About one in 10 people who need such a device actually use them.
However, after hearing this news, many hearing-impaired individuals may run to purchase a hearing aid. According to a study just published by researchers at the Keck School of Medicine at the University of Southern California in Los Angeles, adults with hearing loss who regularly used hearing aids had a 24% lower risk of mortality than those who never wore them.
Hearing loss is very common, affecting an estimated 1·6 billion people around the world, and its prevalence is expected to increase to 2.5 billion by 2050.
The research appeared in The Lancet Healthy Longevity under the title “Association between hearing aid use and mortality in adults with hearing loss in the USA: a mortality follow-up study of a cross-sectional cohort.” The cohort consisted of 9,885 participants, of which 5,037 were female, and 4,848 were male, with a mean age of 48.6 years at baseline.
Dr. Janet Choi, an otolaryngologist and the lead researcher, said: “These results are exciting because they suggest that hearing aids may play a protective role in people’s health and prevent early death.”
New study disproves previous research
Previous research has shown that untreated hearing loss can result in a reduced life span, along with other poor outcomes such as social isolation, depression, and dementia, but until now, there has been very little research examining whether the use of hearing aids can reduce the risk of death.
The new study represents the most comprehensive analysis to date on the relationship between hearing loss, hearing aid use, and mortality in the US, Choi added.
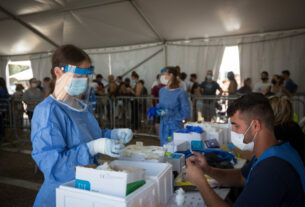
She and her team used the US National Health and Nutrition Examination Survey between 1999 and 2012 to identify almost 10,000 adults 20 years and older who had completed audiometry evaluations, a test used to measure hearing ability, and who filled out questionnaires about their hearing aid use. Researchers followed their mortality status over an average follow-up period of 10 years after their evaluations.
A total of 1,863 adults were identified as having hearing loss. Of these, 237 were regular hearing aid users who reported wearing the aids at least once a week, five hours a week or half the time, and 1,483 were identified as never-users of the devices. Subjects who reported wearing the devices less than once a month or less frequently were categorized as non-regular users.
Researchers found that the almost 25% difference in mortality risk between regular hearing aid users and never-users remained steady, regardless of variables such as the degree of mild to severe hearing loss; age, ethnicity, income, education, and other demographics; and medical history. There was no difference in mortality risk between non-regular users and never users, indicating that occasional hearing aid use may not provide any life-extending benefit.
Regular use of hearing aids might be an indicator that an individual is more health conscious and more likely to follow up with medical appointments. But in this study, the results remained significant after adjusting for relevant factors, including demographics, income, education, insurance, and other chronic illnesses.
While the study did not examine why hearing aids may help those who need them live longer, Choi pointed to recent research linking hearing aid use with lowered levels of depression and dementia. She speculated that the improvements in mental health and cognition that come with improved hearing can promote better overall health that could lengthen the life span.
Choi hopes this study will encourage more people to wear hearing aids, even though she acknowledges that factors, including cost, stigma, and difficulty finding devices that fit and function well, are barriers to use.
She urges that health insurance organizations make additional efforts to improve the accessibility and affordability of hearing aids and to address disparities in hearing health care as evidence of the potential protective role of hearing aid use against adverse health outcomes emerges.
Choi can personally relate to these challenges. She was born with hearing loss in her left ear but didn’t wear a hearing device until her 30s. It then took her several years to find ones that worked effectively for her.
She is currently working on an artificial intelligence-driven database that categorizes hearing aid choices and tailors them to individual patient needs. She also suggests that larger studies be carried out to further understand the link between regular hearing aid use and a lower mortality risk and to promote hearing care.