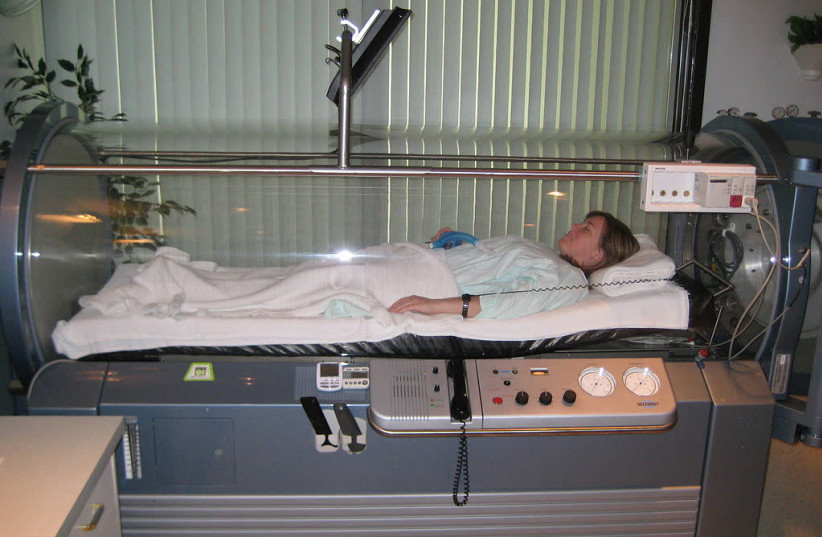
Hyperbaric oxygen therapy (HBOT) is more efficient in treating fibromyalgia that resulted of a traumatic brain injury (TBI) than drug therapy, according to a new Tel Aviv University study.
Fibromyalgia is a chronic pain syndrome from which between two and eight percent of the population suffers. Until about two decades ago, there were physicians who thought that it was a psychosomatic illness and recommended that patients with chronic pain seek mental health care.
Today, it is recognized as a biological illness that damages the brain’s processing of the signals received from the body. When this processing is malfunctioning, you feel pain without any real damage in related locations.
Now researchers at Tel Aviv University (TAU) have compared treatment with a specific protocol of HBOT to drug treatment available today for patients suffering from fibromyalgia as a result of a traumatic brain injury.
The researchers found that the therapy is much more effective in reducing pain than the drug treatment, and it even resulted in the complete recovery of two out of five patients. The comparison was conducted by researchers from TAU’s Sackler Faculty of Medicine led by Prof. Shai Efrati from the Sagol Center for Hyperbaric Medicine and Research at the Shamir Medical Center in Tzrifin and Prof. Jacob Ablin at the Tel Aviv Sourasky Medical Center.
The results of the study were published in the journal PLOS One under the title “Hyperbaric oxygen therapy compared to pharmacological intervention in fibromyalgia patients following traumatic brain injury: A randomized, controlled trial.”
What causes fibromyalgia?
Fibromyalgia can be induced by variable triggers – from certain infections, as we have recently seen in post-COVID patients, through post-traumatic stress syndrome (PTSD) to head injuries.
“We wanted to test whether the new protocols of hyperbaric medicine can provide better results than pharmacological medicine, for patients in whom the fibromyalgia was induced by traumatic brain injury,” said Efrati.
In HBOT, patients stay in special chambers where the pressure is higher than the atmospheric pressure at sea level and where the patients breathe 100% oxygen. It is considered safe, used in many places including Israel and already used to treat a long list of medical conditions. In recent years, scientific evidence has been accumulating that certain newly developed, dedicated hyperbaric treatment protocols can lead to the growth of new blood vessels and neurons in the brain.
In their current study, the TAU researchers recruited 64 Israelis aged 18 and over who suffered from fibromyalgia as a result of a head injury and randomly divided them into two groups. One group was exposed to 100% pure oxygen at a pressure of two atmospheres for 90 minutes (with fluctuations in oxygen during the treatment every 20 minutes), five days a week for three months. The second group received the conventional pharmacological treatment (the drugs pregabalin, which is known under the commercial name Lyrica, and duloxetine, which is better known as Cymbalta).
“The results were dramatic,” Efrati explained. “At the end of the treatment, two out of five patients in the hyperbaric-treatment group showed such a significant improvement that they no longer met the criteria for fibromyalgia. In the drug-treatment group, this did not happen to any patient. In addition, the average improvement in the pain threshold tests was 12 times better in the hyperbaric group compared to the medication group. In terms of quality of life indicators that the patients themselves reported, we saw significant improvements in all the indicators among the patients who received hyperbaric treatment.”
“In terms of quality of life indicators that the patients themselves reported, we saw significant improvements in all the indicators among the patients who received hyperbaric treatment.”
Prof. Shai Efrati
“Today’s accepted treatment for fibromyalgia includes pharmacologic and non-pharmacologic components,” said Ablin. “With respect to the pharmacologic approach, these drugs are not very effective and therefore the emphasis is on the non-pharmacological side – on external correction of pain processing within the nervous system. Currently used recommendations include aerobic activity, hydrotherapy, cognitive-behavioral therapy (CBT) and movement-based therapies such as tai chi. In addition, quite a few patients request treatment with medical cannabis, and for some, it helps. As a whole, existing treatments are not good enough.”
“Fibromyalgia significantly affects the quality of life for people of all ages, and hyperbaric medicine meets an acute need of these patients,” Ablin continued. “Of course, these are preliminary studies, and we must follow and see what effect the medical protocol has on the patients after one, two and three years and if it is necessary to maintain the positive results with further exposure to hyperbaric sessions.”
The research is important because HBOT can heal the damaged brain tissue and not just treat its superficial symptoms, Efrati said.
“In the group that received hyperbaric treatment, you could see the repair of the brain tissue, while in the control group, there was only an attempt to relieve the pain without treating the damaged tissue. Of course, the medication group experienced the side effects associated with drug treatment. This is a difference in approach – to cure instead of just treating the symptoms. We assessed the improvement of the participants in the hyperbaric group more than a week after the last hyperbaric session. More follow-up studies are needed to see the duration of the beneficial effect of the treatment and if and for whom additional treatment will be needed.”
The hyperbaric-oxygen treatment protocol is only available in Israeli medical centers that have licensed hyperbaric chambers. One must stay away from so-called “private chambers” because these can’t provide the therapeutic protocol found to be effective, and they are not regulated and not approved for medical use, the team warned.